On the one hand, deregulating the market for the pill would improve health, lower costs, reduce abortion, and eliminate a political football.
On the other hand, it would reduce incomes for physicians and drug manufacturers, a small passionate minority thinks birth control is immoral, and it is easy to scare the public into resisting change.
Birth control pills are available without a prescription in most countries of the world. Generally most (but not all) rich countries require a prescription as denoted by dark blue on the map and most (but not all) poor and middle-income nations do not as denoted by the other colors.
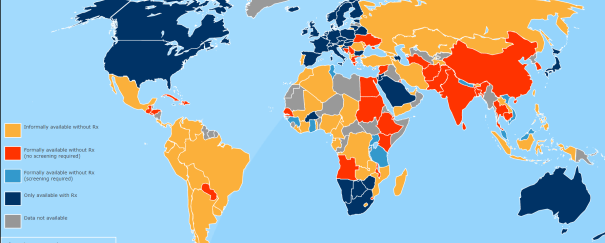
Over-regulated rich countries could learn from our poorer friends abroad. For example, women who live along the US-Mexico border frequently buy their birth control pills on the Mexico side of the border because they are cheaper, more convenient, and don’t require an expensive doctor appointment. As Virginia Postrel says:
Partly because birth-control pills are available only by prescription, people tend to think they’re more dangerous and less well understood than they actually are. In fact, “more is known about the safety of oral contraceptives than has been known about any other drug in the history of medicine,” declared an editorial in the American Journal of Public Health back in 1993. That editorial accompanied an article arguing for over-the-counter sales…. Nearly two decades later, birth-control pills look even safer than they did then, and recent research indicates that women are both able and eager to manage their own purchase decisions.
….Aside from safety, the biggest argument for keeping birth-control pills prescription-only is, to put it bluntly, extortion. The current arrangement forces women to go to the doctor at least once a year, usually submitting to a pelvic exam, if they want this extremely reliable form of contraception. That demand may suit doctors’ paternalist instincts and financial interests, but it doesn’t serve patients’ needs.
….Right now, the American women who have the most choice are those who live near the border with Mexico, where pharmacies sell oral contraceptives without a prescription, generally for about $5 for a one-month supply. A group of researchers [] conducted extensive interviews with more than 1,000 women who live in El Paso, Texas….One result from the El Paso study surprised researchers. “Women who got the pill in clinics were significantly more likely to stop using it during the study — even though they still didn’t want to get pregnant,” Grossman says. That’s a big deal. In fact, he says, “my hope was that we would show that continuation was no worse for the OTC group, but in fact we showed it was better.”

It’s not just doctors who resist making oral contraceptives available over the counter. Pharmaceutical companies usually resist it too. After all, it costs them money for extra testing and produces lower profits at the same time, since OTC meds generally have lower margins than prescription meds. That’s a lot of resistance to overcome.
…another study done in California …compared continuous use of contraceptives among women who got monthly supplies vs. women who got yearly supplies. Over the following 15 months, the women who got yearly supplies were less likely to run out, less likely to get pregnant, and less likely to have an abortion.
Making oral contraceptives available over the counter might be a good idea, but it’s not something likely to happen any time soon. In the meantime, though, providing women with annual supplies instead of making them visit a clinic or refill their scripts every month might have nearly the same benefit. This would require both doctors and insurance companies to change the way they do business, but given the safety of the drugs and the danger associated with running out, annual prescriptions probably ought to be the default.
Although 99% of American women use birth control at some point, many politicians and religious leaders objected to the Obamacare regulation that birth control be covered by health insurance plans. Their objections culminated in the the US Supreme Court’s Hobby Lobby decision. Offering oral birth control over the counter would eliminate the need for them to be covered by health insurance because it would dramatically reduce their cost and increase accessibility. Anna Reisman argues that many other over-the-counter medications like aspirin are more dangerous than birth control and reducing unwanted pregnancy and abortion would do more to improve women’s health than the small risk of adverse side effects that are easily prevented with simple screening done at pharmacies.
[With] the reluctance of religious institutions and hospitals to cover the cost of contraceptive services, the time is ripe for women to make it as easy as possible to get oral contraceptives themselves. The obvious solution is to make the Pill available over the counter. But isn’t that dangerous? Don’t certain oral contraceptives interact in scary ways with other common medications, such as antibiotics? And don’t we need a doctor to help us navigate this complicated maze of information?
Not exactly. First, there are clear guidelines easily available online to determine which women shouldn’t take the Pill at all and which women should have physician oversight. The guidelines are really medical history questions; other than a blood pressure check, a woman can look through the list on her own and determine if she’s a candidate for the Pill. With the combination pill, for example, which contains both estrogen and progestin, women over 35 who smoke and those with chronic medical conditions (including high blood pressure or diabetes, liver disease, specific types of migraines, or a history of blood clots) may be advised not to take the Pill or to take it only with medical supervision. The progestin-only “minipill” can be a good option for women who cannot take an estrogen-containing Pill, since it has fewer risks. User-friendly online guidelines plus a very clear list of risks spelled out on the pill package could make this information easily accessible. Even serious complications such as blood clots and allergic reactions are not a reason not to make the Pill more easily available. Those are extremely rare, and women would have them whether they got the Pill with a doctor’s prescription or not… In many ways having the Pill available over the counter would make it more effective, not less. While the Pill has an impressively low failure rate on paper—0.3 percent in the first year; in practice, the actual failure rate is about 8 percent. One important—and fixable—reason: missed pills and gaps in prescriptions. Some physicians won’t provide a refill prescription unless a woman comes in for an appointment (with some doctors insisting on an often unnecessary pelvic and Pap in many cases). And so for women who can’t get an appointment when they need one, or lack health insurance and can’t afford to see a doctor, or can’t get time off of work to get to an appointment, the story is sadly familiar: missed pills, less effective backup methods, and unintended pregnancies… Pharmacies in metropolitan Seattle have experimented with [one of several models] of “safe use”—the Direct Access study—of making contraceptives available over the counter, in which community pharmacists were permitted to dispense hormonal contraceptives after a woman completed a self-administered screening tool and had weight and blood pressure measurements; both women and pharmacists were satisfied with this experience. Pharmacists already often counsel patients about medications, so it makes sense that they could also play a key role in helping women choose whether an oral contraceptive over the counter would be a good option.
Fortunately, some states are starting to deregulate the market for hormonal birth control:














Leave a Comment